Gum Graft/Transplant for Dental Implants… Is It Necessary? IT IS ONE OF THE KEYS TO SUCCESS!
When talking about dental implants most people focus on the bone alone. The bone sets the tone, but the (gum) tissue is the issue. I get 100s of questions asking if a gum graft should be done at the same time or if I can fix an implant that has threads exposed on the outside.
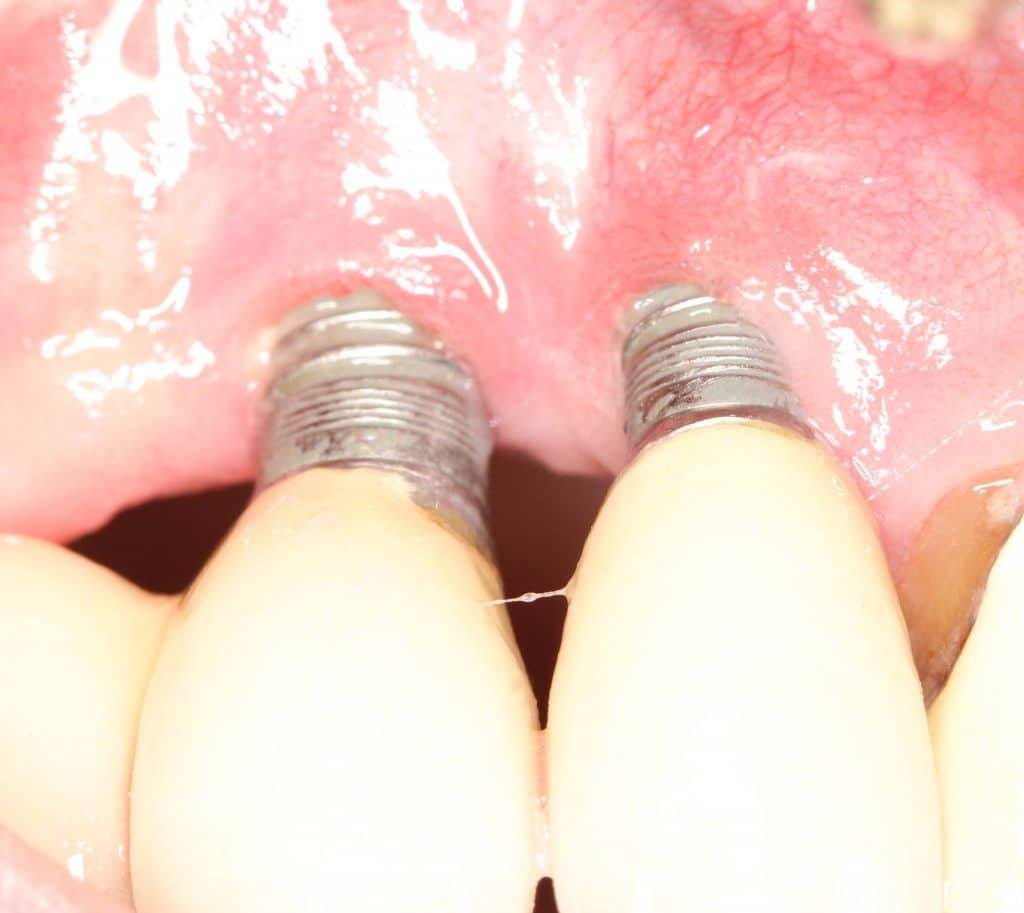
There are different kinds of gums in your mouth. There is tight, durable and firm gum tissue. Then there is loose gum tissue that is called “mucosa.”
Why is it important to have gum around an implant?
Having more gum is ALWAYS better than less gum tissue.
Think of it like this. On the palm of your hand that skin is very durable because it contains a lot of keratin. You can beat up your hands and they do not start bleeding and peeling. Imagine if you had the skin on the inside or outside of your eyelids on the palms of your hands! You could imagine that your hands would be in pretty bad shape!
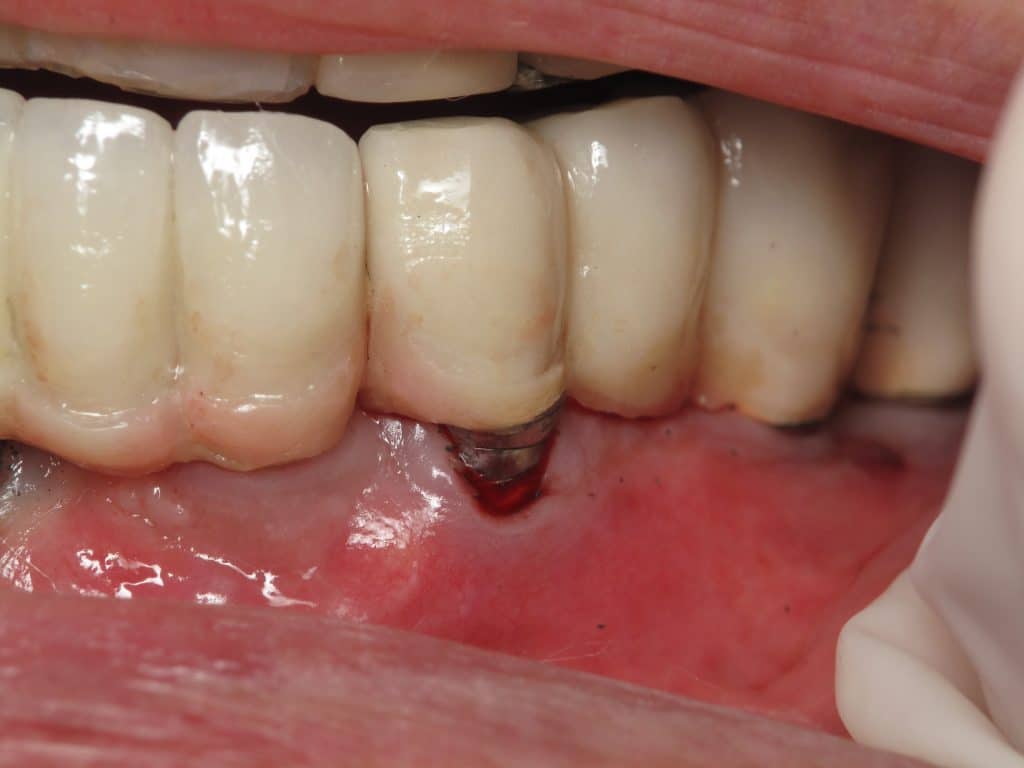
Not enough gum around an implant
If you do not have enough gum tissue you will notice that the gum recedes around your implant causing pain, inflammation, and the threads of the implants will become exposed. Even simple tooth brushing will cause the gum to recede away. As the gums recede away, the bone will as well causing peri-implantitis/peri-implant mucositis. These are chronic conditions that almost always lead to permanent implant problems and likely implant loss.
Prevention: This is prevented by planning for this to happen and knowing the diagnosis of your anatomy !!!!!! keep in mind that some people have genetically thin and genetically thick gum tissue. Just like hair some people have more than others!!! Some people have extra muscle “frenum ” that pulls on the gum constantly… Eventually pulling it off the tooth or implant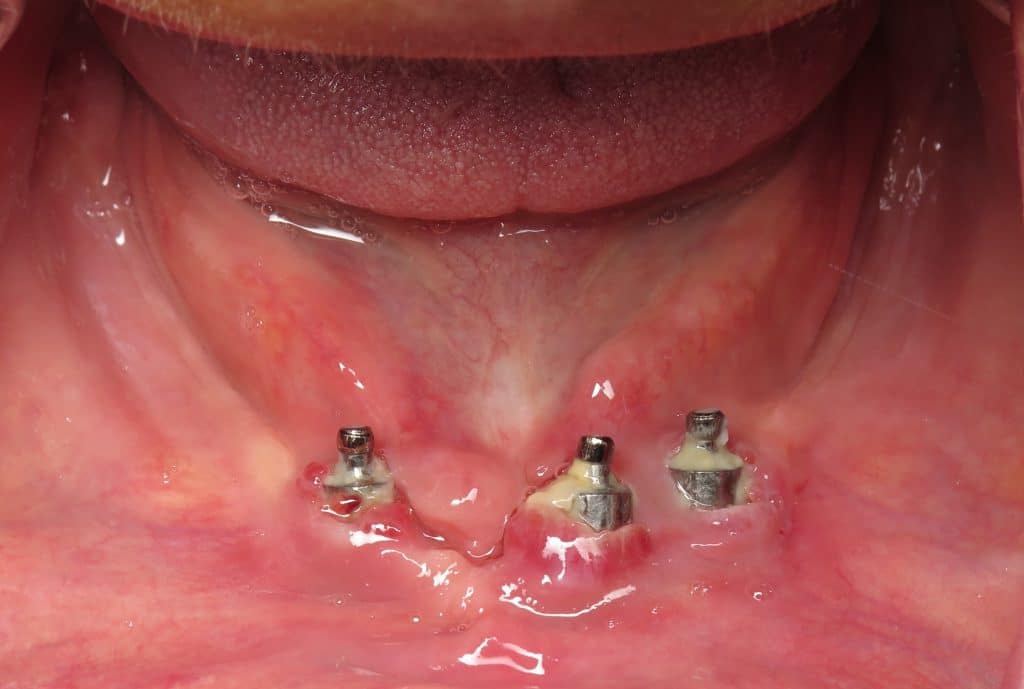
If you do not have enough gum tissue At the time of surgery this can be corrected by borrowing gums from the inside part of your mouth and just moving it to the outside. I call this an apically positioned flap …just relocating good gum into the areas of bad gum. I do this every day. This is by far the best, easiest and cheapest approach. It needs to be done at the time of surgery typically before the dental implant crown or bridge is put on. Often times the frenum needs to be cut as well so that it no longer pulls.
They can also be corrected by taking gum from the roof of your mouth either behind your upper wisdom teeth or right on the palate and stitching it onto or under the gum of the implant.

Recession happens because of trauma or plaque. Brushing your teeth too hard is trauma, bad crowns or fillings also cause gum recession. It also occurs on people with a shallow cheek pouch vestibule. The connective tissue with in our gums provides a strong defense against inflammation. If the gum around your implant becomes inflamed it will feel painful, sensitive and look red.
Gum recession affects up to 88% of people >65 yrs // 50% of people 18-64 yrs on their natural teeth. If you start off with thin gums then they may only get thinner with implant treatment. It is best to plan for progressive thinning so that you do not lose your implant.
Bottom line is having a gum graft or gum repositioning surgery will always help prevent problems. In my clinical practice I am always repositioning gum tissue or taking from one area and transplanting to another. I do not want to see my patients end up with problems. Basically implants have to be over engineered with bone and tissue to make them last as long as possible since they are not permanent.
This is a complicated topic for sure!
Ramsey A. Amin, D.D.S.
Diplomate of the American Board of Oral Implantology /Implant Dentistry
Fellow-American Academy of Implant Dentistry
Burbank, California

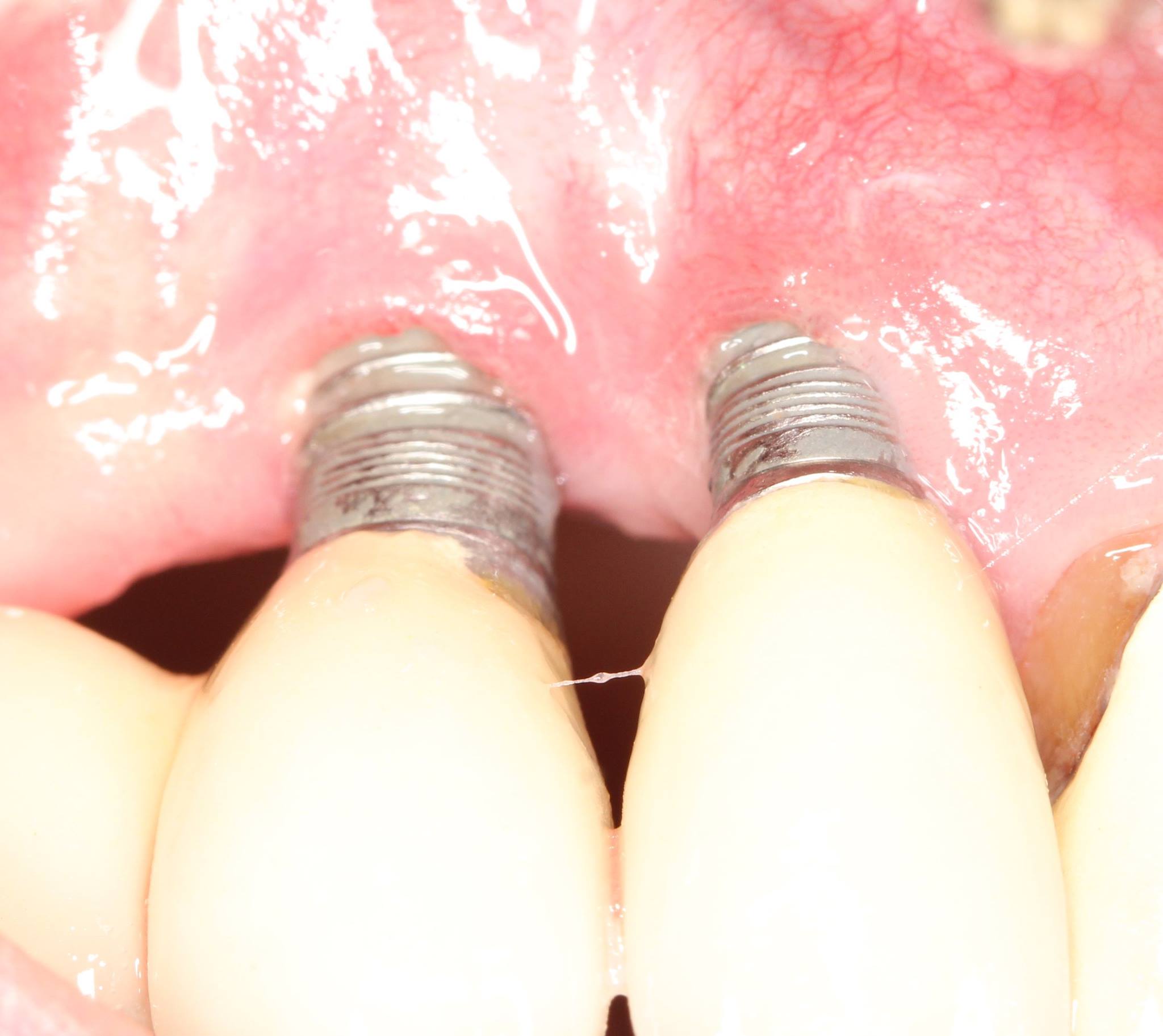
I have an implant on #19 and my gums are starting to recede around the implant. can I get gum grating around the implant?
Maybe. It depends on if the bone is lost as well.
Hello. I am congenitally missing the two teeth either side of my top middle teeth. I recently had titanium implants, and my permanent crowns have been placed. I went to a reputable oral surgeon for the implants and a prosthodontist for the crowns. I thought the final abutments were going to minimize the dark grey look underneath my gums directly above the teeth. I still notice the dark grey and am bothered by it. Would it be possible to do a gum graft to make the tissue thicker/denser to cover the grey? Is there anything that can be done? I am about two weeks out of getting the final crowns, and the gums between my teeth are still forming. I am 21 years old, female. Thank you.
Yes-adding gums would help this. Because you were not born with these teeth become an bone is always thin in this area. It can be done through a tunneling technique. I have done this many times.
Dr. Amin, you said “Having more gum is ALWAYS better than less gum tissue” in your article. However, my dentist who is to place a permanent crown for my implant (not in front but very end) wants to cut (‘shape’, ‘surf’) some of my gum tissue around the implant. He said this is needed because the implant (a small cylinder) allowed a large amount of gum tissue that is too much for the permanent crown (bigger, as a real tooth), and removing some gum tissue would prevent food from being stuck within the gum, potentially causing infection. What would you say to my dentist? Thank you for your answer in advance.
This is a great question. It is always great to have extra gum because you can trim it away if needed! This means you are in a great situation to have a successful single tooth dental implant!
Hello, can you get gum grafting done prior to getting an implant? Will gum grafting prior to getting a tooth pulled for an implant be useless? Is the gum grafting better done after the implant is finished?
It is always best done before or during implant placement rather than after.
Dr Amin-I cannot begin to say how helpful your comments on dental problems are-I wish your office was near me ( NJ ) One side , bottom left – my gums are a little bumpy compared to the others which leads me to believe their is thinning of the gum in that area. They have not pulled away, still up to the tip of the teeth, though I do have a three crowns and one root canaled tooth. Fanatical about caring for my teeth since the root canal a couple of years ago-always brush gently after meals, floss, oil pulling, essential oils, salt rinses, beneficial non alcohol mouthwash, etc. I even gave up snacking in between meals. soda, etc. My gums are a good pink color and healthy , but I am 62 and getting to an age where thin gums present problems. Can an alloderm or mucoderm patch be placed on the outside , or does it always go in the inside? My gums are tight-I cannot even think how they could be cut open and something placed inside. I know palette tissue is better but I would rather not use that -. So I also looked into emdogain as well-some see it as beneficial , others not so much. Trying to research gum regrowth and tooth regeneration and its always just around the corner, but just not here yet-( Mao, Sharpe. Lauster, Tsjuli ) What are your thoughts on how close we are to these problems and do you think a collagen graft or alloderm with emdogain would be successful? Sorry for the long post
Hello Dr.Amin,
Thank you so much for your time . I’ve had #18 ( the second molar I believe )extracted 15 years ago so there is a noticeable dip in between the teeth. The periodontist and 2 oral surgeon said that I have enough bone to support implant regardless of visible concave between tooth 19 and 17. My dentist however asked that I get a bone graft to make the tissue even with the adjacent teeth to prevent a “ food trap “. The two surrounding teeth have also shifted and 19 is leaning inward . He said he may have to slightly shave down the adjacent teeth for a better fit . He uses Zimmerman biotmet and lectures/ consults for them quite a bit. Are they as reliable as strauman in your opinion ?
When I consulted with the periodontist after the request for a bone graft from the dentist she reiterated that I did not need one and that she could bulk the concave with gum tissue instead . She said that she would use gum from the roof of my mouth or,that she could use gum that comes in a pack . Is this a good alternative? Also, would she be able to place the implant at the same time as the gum graft ? Also, is there ever an option to fill bone inside of the gum graft ? I just realized I asked you like 10 questions in one .Thanks again for your time . Stay safe and healthy
Replacing 18 when 17 is being kept is complex. Read this article about second molars and stay safe as well!
I am 29 years old and eventually going to have to get implants for front two teeth. When I was 8 years old (21 years ago) I fell on the concrete and hammered my two front teeth back up into my gumline. They came back down on their own and were bonded while I had braces and several other contraptions to widen mouth and correct jaw. Then when I was 18 I had two crowns placed on front two teeth, then couple of years later ( age 24) I developed a gum fistula above on of my front teeth and had root canals in front two teeth along with apicoectomy , after I had two new crowns then veneers on the two teeth beside my front teeth. Here I am five years later another small gum fistula, but teeth and gums look perfect, no pain, no swelling, no redness, but I am told the x ray shows infection. I am scheduled to have apicoectomy along with a bone graft, but I am told this is only buying me time until I have to get implants. I am worried about what implants will look like…my teeth are perfect now…I’m devastated. Will having two apicoectomies affect my bone structure for future implants? I also have a high smile line.
This comment went to spam –sorry. How did it go?