Here is an interesting full double arch dental implant case that I took over from another dentist. This patient desired full mouth dental implants. When he presented to my office he already had 10 implants but could not use his teeth. He paid a lot of money only to be disappointed with the removable over dentures that were made for him.

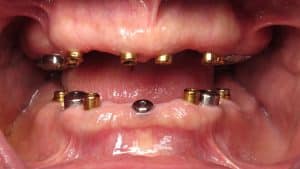
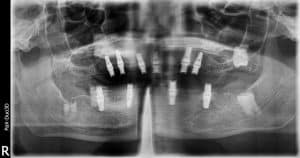
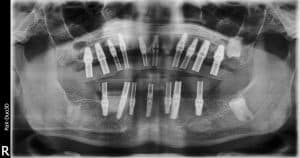
You can see on the preoperative x-ray that he had 6 upper dental implants and only all on 4 lower dental implants.
The implants were mostly well placed from a spacing standpoint and might have been able to be used for fixed dental implants such as a Prettau zirconia full mouth dental implant bridge. Rather than having a fixed bridge or an all on 4 fixed bridge, the dentist chose to make an overdenture!!
The overdentures never worked for him.
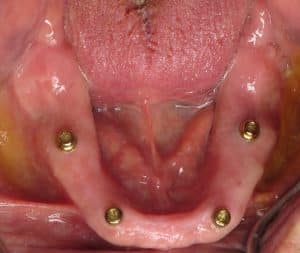
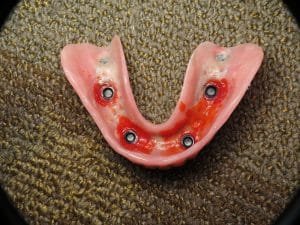
They were way too bulky and had a tremendous thick pink area we call a flange. The crazy thing is that there is no way overdentures could have ever worked because all the implants were placed way too shallow! In order to have overdentures, you must have enough room from top to bottom (inter-arch space) to fit the dentures and plastic abutment attachments that make them snap into place. The gold attachments are called locator abutments which typically work well on the lower jaw only.
He never wanted to have removable teeth but that is NOT what he got. He was not able to wear the overdentures at all and came to me for a better solution. He had gone 3 years like this. The teeth were even made twice and then he gave up. He told me I was his last hope.
After evaluating him carefully I determined that the implants were placed in a shallow position more ideal for “regular implants.” We refer to this in dentistry as an “Fp1” prosthesis. That means there is no reason or room for the pink portion which most patients need because they are missing bone and gum. This patient actually had excessive bone which is very rare and in retrospect if he really wanted an overdenture should’ve had a bone leveling alveoloplasty procedure.
This very well could have been a communication problem between the restorative, tooth making dentist, and the implant surgeon. In this case, there were 2 different people who started the procedure. I am a strong believer that these complex dental implant procedures should be done from start to finish with a *single* skilled provider or a very tightly connected and experienced partnership duo.
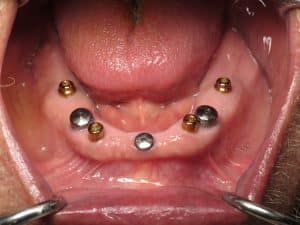
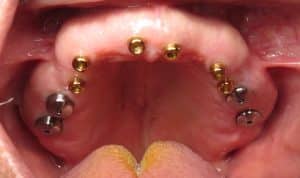
The upper implants unfortunately were all squished in the front, without any dental implants in the molar back tooth positions with minimal inter-arch space. On the lower jaw they were well spaced but there was too much space between implants for the regular/crown and bridge/Fp1 type teeth.
The solution was to add four additional implants into the molar regions on the upper with some simple internal sinus lifting. On the lower jaw I added 3 implants in strategic locations to shorten the spans of the bridges. If the span is too long, and the zirconia material is not thick enough, the teeth will break…yikes!!!! The additional implants will support the material. This will allow him to have basically regular teeth back again without any of the pink porcelain or pink plastic.
In a single appointment, I added these additional 7 implants with minor sinus grafting under IV sedation at my office in Burbank, California. The implants were allowed to heal for approximately 4 months prior to starting the restorative process.
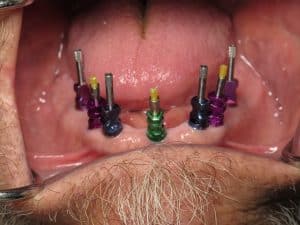
Fabricating his teeth was very complex because of 2 different implant systems and at least 4 different proprietary screwdrivers and parts. The locator abutments also had a very narrow “sulcus” which would be too small at the tooth neck for regular size teeth. I actually had to custom alter make all of the special titanium implant impression transfers to fit into the overly narrow gum channels.
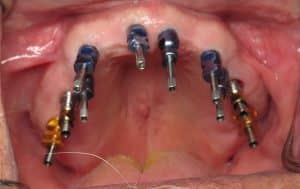
A verification jig was 3D print milled to be certain that all 17 implants had a very accurate impression so that there is no misfit of the new teeth. I also created a screw retained wax rim teeth in order to select tooth size, color, position, bite level and a host of other factors.
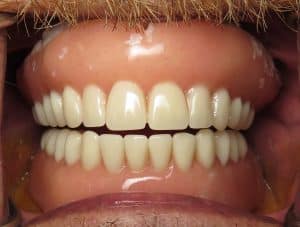
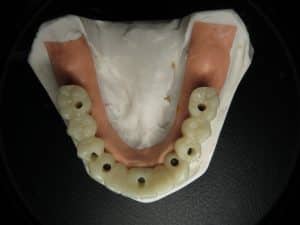
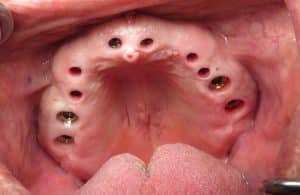
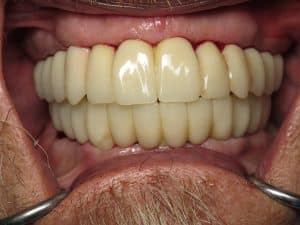
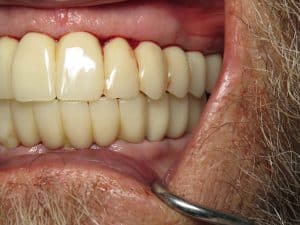
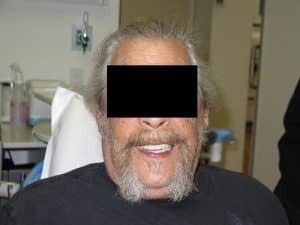
In these photographs what you are seeing is a temporary PMMA double arch bridge. This is not the final although it may look like a final bridge!
All teeth were designed using 3-D 3shape software. I had my very skilled lab technician digitally create wider gum channels so the teeth at the neck appeared more of a normal size so they would not have mushroomed stalks. At the delivery appointment for the temporaries I had to surgically open his gums to fit the teeth. This will allow any papilla or gum triangles to fill in as needed and “groom the gum tissue” to fit the new teeth. The PMMA is a milled plastic/acrylic material so the bite can be adjusted and refined. I will then take all of this information and translate that to the final restoration.
I usually allow my patients to wear the screw retained PMMA full fixed implant temporary bridge for a few weeks to a few months depending on how much testing and adapting the patient needs. Some people adapt very quickly with speech while others need a bit more time to learn where there teeth are in space. This testing duration also allows the TMJ jaw joints an adaptation period. Also the bone can progressively be given bite strength with this softer material and gradually get to the solid monolithic zirconia restorations.
Sorry for the blood in some of the photos as they were taken on the day of surgical delivery of these temporary restorations. The finals will look very similar to this except even better 🙂
I hope this explain some of the highly complex procedures that go into recovering such a difficult situation. Unfortunately a lot of what I do nowadays is correcting and redoing bad situations which could’ve been done right the first time with better planning.
Ramsey A. Amin, D.D.S.
Diplomate of the American Board of Oral Implantology /Implant Dentistry
Fellow-American Academy of Implant Dentistry







I’m 41; due to loss of enamel, most of my teeth having crowns, and the need to re-crown, I had two dentists advise me to have all of my teeth extracted and replaced “with implants.” The second dentist explained I wouldn’t have 32 (or 28) implants – I would have a few implants and either “snap-on overdentures” or “fixed bridges.” I wanted the fixed bridges, but cost is an issue. I asked my surgeon if implants could be done so that I wore an overdenture for a couple of years, then transitioned to a fixed bridge. He said the implants would be done the same, so I would be able to transfer to a fixed bridge with no additional work by him. It made sense to me, until after surgery 2 weeks ago. Your article states, “The upper implants unfortunately were all squished in the front, without any dental implants in the molar back tooth positions with minimal inter-arch space.” I’m not sure about “inter-arch space,” but I do know the implants are “squished in the front.” Front-to-back, I see “implants, implants, several holes.” Almost like he implanted 4 front teeth. Regardless of overdenture vs bridge, my concern is the same: trying to chew a steak with my molars and the prosthesis either snaps in half or snaps off. Should I have implants placed in the molar region before even getting the overdenture in 6 months? Thanks for this well-written article – I feel like my concerns are justified.
Thank you for your kind words. Yes you need implants in the back. Transitioning from an overdenture to a fixed bridge requires an expert in implant dentistry. Do your due diligence!
I had G4 by Golpa, all teeth removed 5 days ago and full upper and lower hybrid bridges installed 4 days ago, yet still lots of swelling, black and blue cheeks, and pain five days later. Here is my question, I feel as if the TOP bridge has a design flaw because i can feel the teeth pushing into my inside cheek, as if the top bridge was made to wide on the left and it is protruding outward. I have high pain tolerance, I am very athletic and healthy so my recovery should be good. But i believe whoever made the top bridge messed up. What to do, any thoughts? My concern is that the dentist came off as not the perfectionist type who tends to play down concerns because he has to keep the patients moving along the conveyor belt so to speak. I live a five hour drive from the office but i am tempted to drive back tomorrow to have this addressed because they will be closed for the entire weeks of Christmas and New Years. Your thoughts would be appreciated!
I hope it is not the final! Best to have provisional first. Have the temp made again would be the best advice. Unfortunately that place is a factory just churning things out rather than customized.
You wrote “have the temp made again.” I agree with you, my bridges weren’t made or fit properly and are causing feelings of pressure and pain. They said they could remake new PMMA’s tomorrow — Thursday and inserted on Friday — “if I insist.”
I will tell the doctor to work with his lab tech to make sure all measurements are correct this time and the new temps are crafted accurately. QUESTION: If the doctor claims it is too soon to remove and replace the temporary’s since all teeth were extracted and posts installed on 12/09/20 and full upper and lower bridges installed on 12/10/20, is that a legitimate concern, is it too soon to do this on 12/17 and 12/18/20?
(PS- they are closed for two weeks after 12/18/20 and I cannot tolerate waiting till into 2021, I live five hours away and came back today, staying at hotel to have doctor address this now, I dont even care about the smile, it is these two boulders inside the back of my upper mouth crafted poorly that are killing me, please doctor time is of the essence and I am in dire need of your response to my question before i see the doctor at 10:00 AM EST on 12/17/20 Thursday, thank you again for your time and consideration)
It is fine to remake the case this early but only as temps! As long as the implants are solid this will be ok. If they were not that tight in the bone there is a big risk. Good luck!
Thanks Doctor. Today 12/17/20 I was examined by the Dentist at Golpa and he agreed that the upper bridge was made way to wide with the teeth protruding out in the back — going into my inner cheek. So he brought his lab tech into the room and showed him the problems and they are making new upper and lower bridges. I will return tomorrow 12/18/20 for the dentist to install the new bridges. Hopefully they are better customized, a better fit. How would I know if the implants were solid? They were put in on 12/09/20. Would implants be tight in the bone 8 days after they were put in? The dentist said he would prefer to leave the original bridges in for 2 months to integrate but he did acknowledge that the top bridge especially — was way too wide for my mouth and I felt the pressure and pain would have been too debilitating to endure for two months. He made me sign a release…yet they messed up by building bridges that were too big, a very poor fit that were NOT functional, nice smile aesthetically but if the bridges are poor on functionality it almost makes you not care about how nice your smile is and has one yearning for their old crummy crooked teeth. In 2020, with todays technology this should not have happened. Someone was sloppy and their lab tech and dental surgeon were not in synch, the way you and your lab tech are. Either I had a bad luck of the draw, or this happens more via Golpa offices then is reported. I have read the dentists credentials, he is more then capable to do the job right the first time and he is highly trained enough to correct bad issues when they arise. Hopefully that will be the case from here on out. The new bridges they install tomorrow are PMMA/Titanium and they tell you to come back in 6 months for mandatory examination and at that time you can keep what you have OR you can upgrade to G4-High Class Nanoceramic Trilor for an additional $9000.00 . If I am happy after 6 months with the PMMA/Titanium why would I not keep them? (PS- if I had to do over again — my suggestion to people considering implants — I would have gone to Dr. Amin and not a factory that churns out ill fitting bridges with their focus on seeing volume rather then emphasizing customization like Dr. Amin does)
can a fixed bridge implant use the same screws that a previous overdenture used? Or do those screws have to be replace?
yes…if it was planned this way and/or if the implants are at the right level. Almost always if the bone was leveled flat. I hope so!
I am wondering IF a person has gotten an over denture, is it possible in the future to get a fixed implant bridge attached to the screws that held the over denture in place? ( or are the screws that held the over-denture in place too short or shallow?? I am confused… Please advise. God bless you for this website of yours
please see other reply 😉
I am having all of my upper teeth pulled in the next week. I have requested having fixed full arch implant bridges, but my dentist is trying to talk me into having a removable “over denture” instead. He says it is a much better option, because a non removable implant bridge is harder to “clean around”, and is expensive because the dentist will need to do cleanings, etc. Please shed some light on this for me. I am grateful for any advice you can share..
No!!!!!!!! Fixed is way better as long as designed properly and tested with temps!
I just got 12 implants, 6 on the bottom jaw and 6 on the top. I was under the impression that I would be getting bridges but just found out I am getting snap-in over dentures, and am pretty bummed about it. I just wanted to know if it’s possible to later on get fixed bridges with the implants I already have?
WHAT!!!!!!!!!!! Why not stop now and do it right with fixed zirconia bridges. It sounds crazy to spend all that money to end up with something removable. You have plenty of implants to do fixed!!
I live in NC and in the early stages of investigating options. Missing about 8 teeth and have a few loose teeth and it was recommended that they come out. Obviously, bone and gum issues need to be resolved before considering a fixed bridge solution. Is there anyone in NC you could recommend that might allow me to get what is needed under one roof? I’m in the Charlotte area.
Thanks, Ray
I had a subperiosteal implant done in the mid 90’s It’s more like a plate and I’m wearing a snap on overdenture. Can this be converted to a periosteal implant with a fixed bridge?
Yes definitely. It will take somebody with a very advanced skill set to be able to treat you. If it isn’t upper jaw you may require zygomatic dental implants if there is very little left
Hello dr. Amin, I have a subperiosteal implant about 12 years now but just found out from recent dentist visit ( new dentist my old one past away) that my upper imp,ant is infected so they told me it has to be removed ASAP , my concern is, if I have this implant remove Will I be able to get another fix bridge implant? I know that I have no ridges or gum not even a bone what’s is your advices? The dentist in my area had told me they can’t help me I’m getting so depressed since finding out my situation .
subperiosteal implant is great for the lower jaw. It does not have as good of a success for the upper jaw long-term. You should consider seeing somebody who is well trained in zygomatic implants to retreat your upper jaw if it has to come out. I’m sorry for your troubles ;-(
I have full upper and lower snap- in dentures-4 implants top and 2 bottom. For the last 2 years Ive had several
please finish your post
For the last several years I’ve had teeth individually snap off both the top Appliance and bottom. What can I do to prevent this?
That’s the nature of acrylic over denture teeth. I would suggest you upgrade as this post is discussing to fix bridgework. Search “prettau” on my site for more info and see links in this post.
I just received my upper all on 4 hybrid denture in the roof of my mouth the acrylic was sharp and on both sides I was biting my cheeks he removed some of the material and polished my denture which helped some on the biting of the cheeks but when he polished the roof part I now have a big gap and when I talk I talk through my front teeth sounds like I have dentures he told me that they would be screwed in and cemented over the screw the he tells me that snap on is a better way to go my right side fits well teeth line up with bottom teeth and have less pink material feels great with my tounge on the left side it is thick and teeth don’t line up the upper plate flexes when I bite down the left side that doesn’t line up has some pain I complained about the material he removed on the roof of the plate and he said that when he polished it probably removed to much but you are stuck with it I hate the way these teeth feel in my mouth but people say you will get used to them and the Dentist told that when you bite your cheek it will get tough should I complain more or seek another Dentist.
I am hoping that this is just a temporary restoration for you. I would hope that you are not being provided the final restoration on the same day of surgery. Routinely I provide same day all on X implants and provide same-day immediate teeth but these are just temporary. There is no way to work out all the details for aesthetics, phonetics, bite all on a single day surgery. After healing for a few months with the temporaries, I will convert patient to final solid zirconia Prettau Bridges. Here is how the process works on the lab design side. none of this is done for the same-day procedure until the gums and bone have healed enough. Hang in there and in the meantime be sure to stay on a very soft diet.
I HAD THREE MISSING TEETH, THAT WERE ROTTED-OUT AND PULLED AFTER BEING FIXED,TWICE, MY ORAL AND FACIAL DENTIST WANTED ME TO PUT DENTAL-IMPLANTS,IN RIGHT AWAY. I DIDN’HAVE DENTAL INSURANCE AND TOLD HIM, I COULD’N DO THIS NOT @$ 2,600 PER
TOOTH, ITS BEEN ABOUT 2-YEARS NOW AND I HAVE BEEN IN THE HOSPITAL EMERGENCY ROOM
TWICE NOW SCREEAMING @ THE TOP OF MY LUNGS WITH LEFT-JAW PAIN THINKING I WAS HAVING A HEART ATTACK, THEY TOLD ME NO I WAS’NT,WENT BACK TO MY DENTIST AND HE NUMBED MY LEFT-JAW, JAW PAIN WAS STILL THERE,HE SAID I HAD TMJ, SAW THREE-DOCTORS,
ABOUT THIS GAVE-ME PAIN PILLS.3-22-2017 I LOOKED IM MY OWN-MOUTH,GUM-LINE BELOW THE
CHEWING-TEETH, I HAVE JAW BONE ATROPHY,GETTING WORSE,GOD-BLESS YOU FOR ARTICLE
SHOWING HOW YOU WOULD FIX-THIS. MY DENTIST-ORAL FACIAL REPAIR,TOLD ME NOTHING
ABOUT WHAT WAS GOING TO HAPPEN TO ME ,IF I DID’NT GET THE TEETH-FIXED,YOU ARE A ANGEL FROM HEAVEN,FOR PUTTING THIS ARTICLE,WITH PICTURES, ON HOW TO FIX THIS PROCEDURE. “god bless you” always
You have shared here almost every aspect of bad dental implants and the good impact of full arch bridges. But I want to know that is it possible in every case?
Every case is different and unique. There is no cookie cutter response to every problem. I treated every patient as individual and work towards a proper diagnosis and then an appropriate treatment plan.